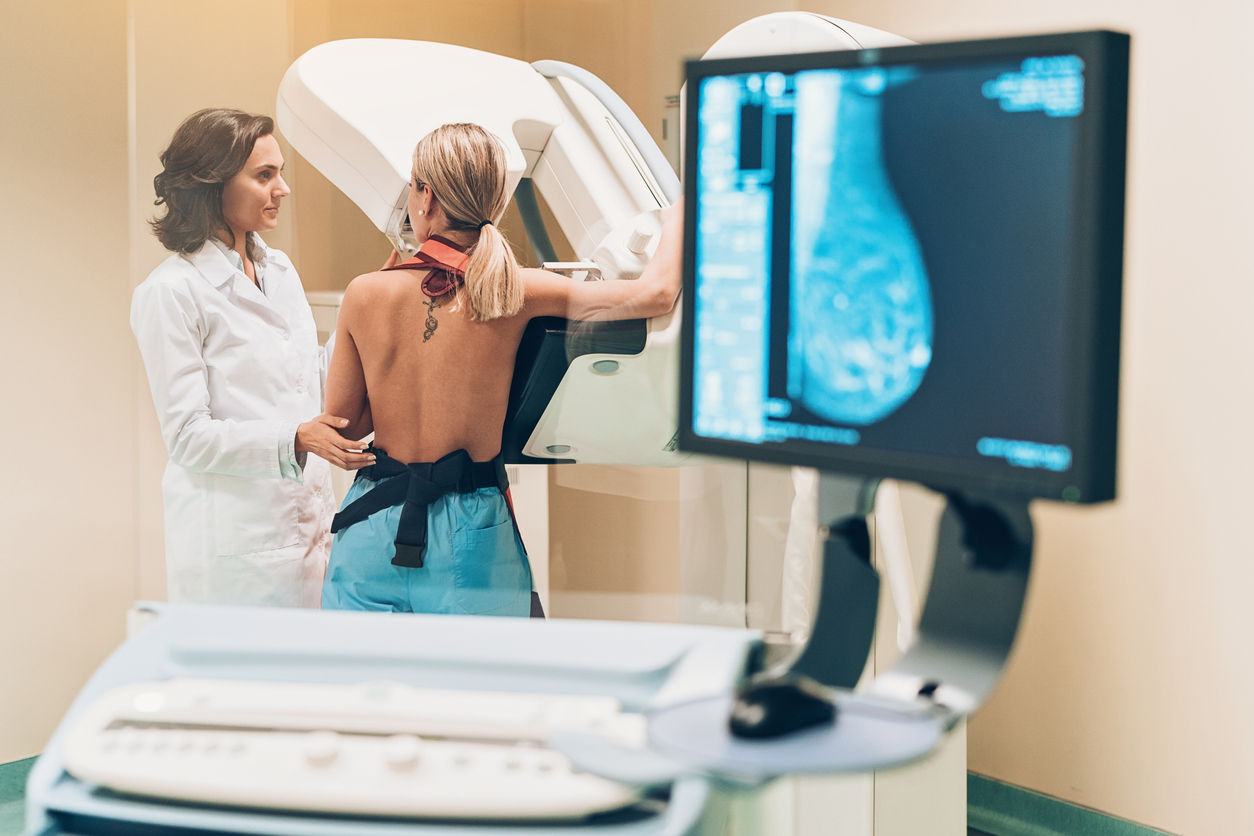
Breast cancer screening plays a significant role in detecting cancer early, often before symptoms appear. Early detection of breast cancer allows doctors to use more effective treatments and achieve better outcomes.
Today, doctors use several imaging tools to examine breast tissue and identify abnormalities. Each type of screening test offers different benefits, and physicians may recommend one or more imaging methods depending on a patient’s age, personal risk factors, family history, and breast density.
This guide explains the most common breast imaging tests, how they work, and when they may be recommended. Understanding these screening tools can help patients feel more informed and confident when discussing breast health with their healthcare provider.
Why Breast Cancer Screening Matters
Breast cancer is one of the most common cancers among women, but early detection greatly improves survival rates. Screening allows doctors to identify cancer before it causes symptoms or spreads to other parts of the body.
Many breast cancers are first discovered during routine imaging exams rather than through physical symptoms. According to the American Cancer Society, mammograms can detect tumors years before they can be felt during a physical exam.
Detecting cancer early often means:
- Smaller tumors
- Less aggressive treatment
- Better long-term outcomes
Regular screening is one of the most effective ways to protect breast health. Patients should follow recommended screening guidelines and discuss their personal risk factors with their doctor to determine the best screening schedule.
Mammograms (Standard Breast Screening)
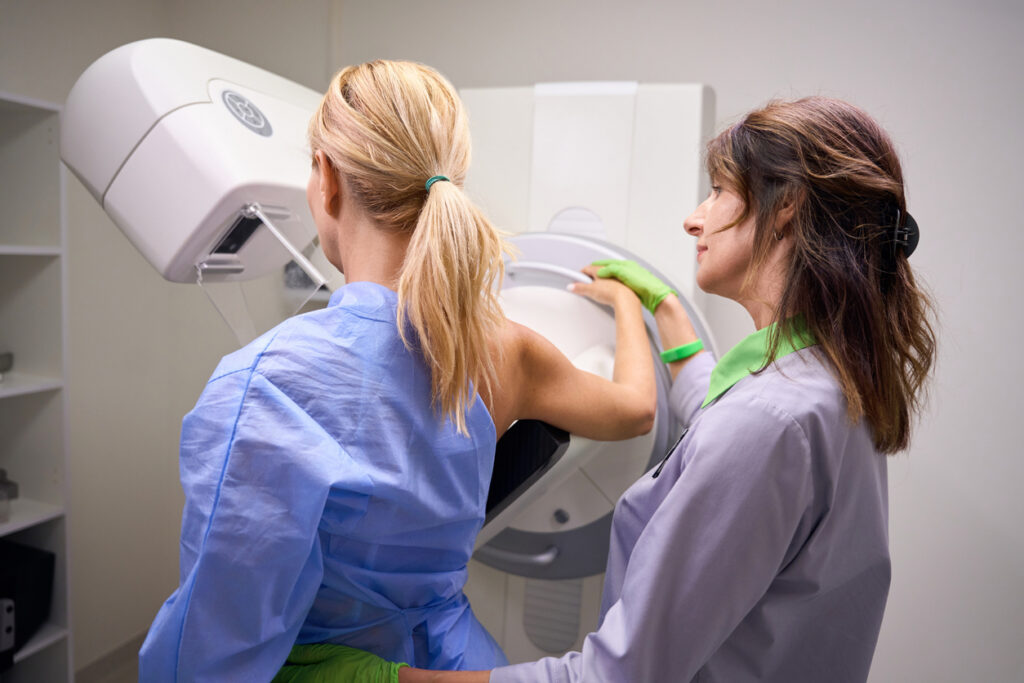
What Is a Mammogram?
A mammogram is a specialized medical imaging test that uses low-dose X-rays to examine breast tissue. It is the most widely used and recommended screening tool for detecting breast cancer.
Mammograms can identify small abnormalities such as masses or tiny calcium deposits that may indicate early cancer development.
When Mammograms Are Recommended
Most major medical organizations recommend that women with average risk begin regular mammogram screenings around age 40. Screening frequency may vary based on individual risk factors and physician recommendations.
Doctors may advise earlier screening for women with a higher risk of breast cancer. This includes those with a strong family history of the disease or other risk factors.
What to Expect During a Mammogram
A mammogram is a quick and routine procedure. During the exam:
- The technologist positions the breast on a special imaging platform.
- A compression plate gently presses the breast tissue to spread it evenly.
- X-ray images are taken from different angles.
The compression lasts only a few seconds and helps produce clearer images while reducing radiation exposure.
Most mammogram appointments take about 20 minutes, though the imaging itself usually takes only a few minutes. Results are typically reviewed by a radiologist, and patients receive their results within a few days.
3D Mammography (Digital Breast Tomosynthesis)
How 3D Mammography Works
3D mammography, also called digital breast tomosynthesis, is an advanced form of mammography. Instead of capturing a single image of the breast, the machine takes multiple X-ray images from different angles.
These images are then combined to create a layered, three-dimensional view of the breast tissue. This allows radiologists to examine the breast one thin layer at a time.
Benefits of 3D Mammography
3D mammography offers several advantages compared to traditional mammography:
- Improved detection of small cancers.
- Greater accuracy in identifying abnormalities.
- Reduced need for additional imaging tests.
- Better visibility in dense breast tissue.
Studies show that 3D mammography can reduce false positives and unnecessary callback appointments.
For many patients, especially those with dense breast tissue, 3D imaging can provide clearer and more detailed results.
Breast Ultrasound
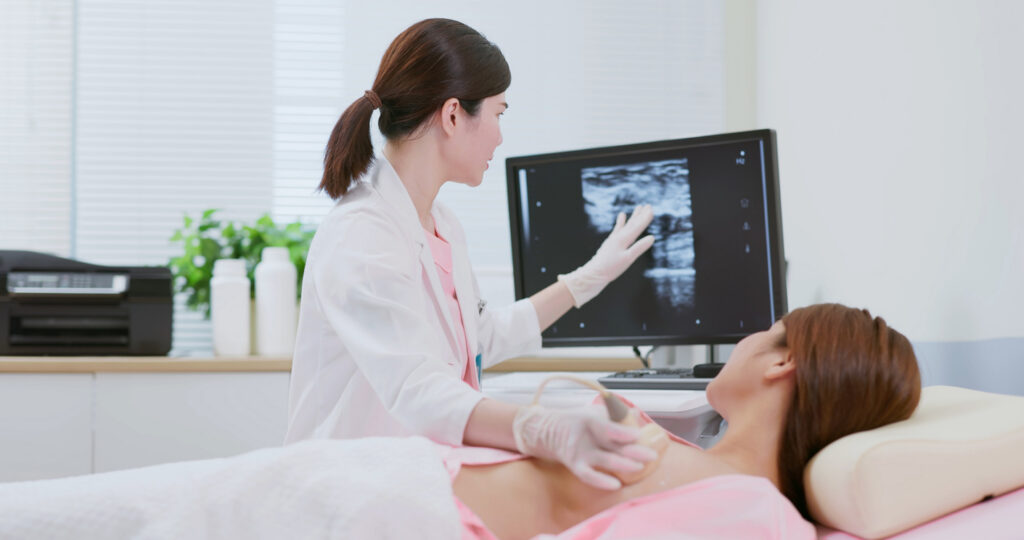
What a Breast Ultrasound Is
A breast ultrasound uses high-frequency sound waves to create images of breast tissue. Unlike mammograms, ultrasound imaging does not involve radiation.
A handheld device called a transducer is placed on the skin, sending sound waves into the breast. These waves bounce off internal structures and produce images on a monitor.
When Breast Ultrasound Is Used
Doctors commonly use breast ultrasound as a supplemental imaging test rather than a primary screening tool. They may recommend an ultrasound:
- To evaluate an area of concern found on a mammogram.
- As additional screening for women with dense breast tissue.
- To determine whether a lump is solid or fluid-filled.
Ultrasound is particularly useful for distinguishing between cysts (fluid-filled sacs) and solid masses.
Breast MRI
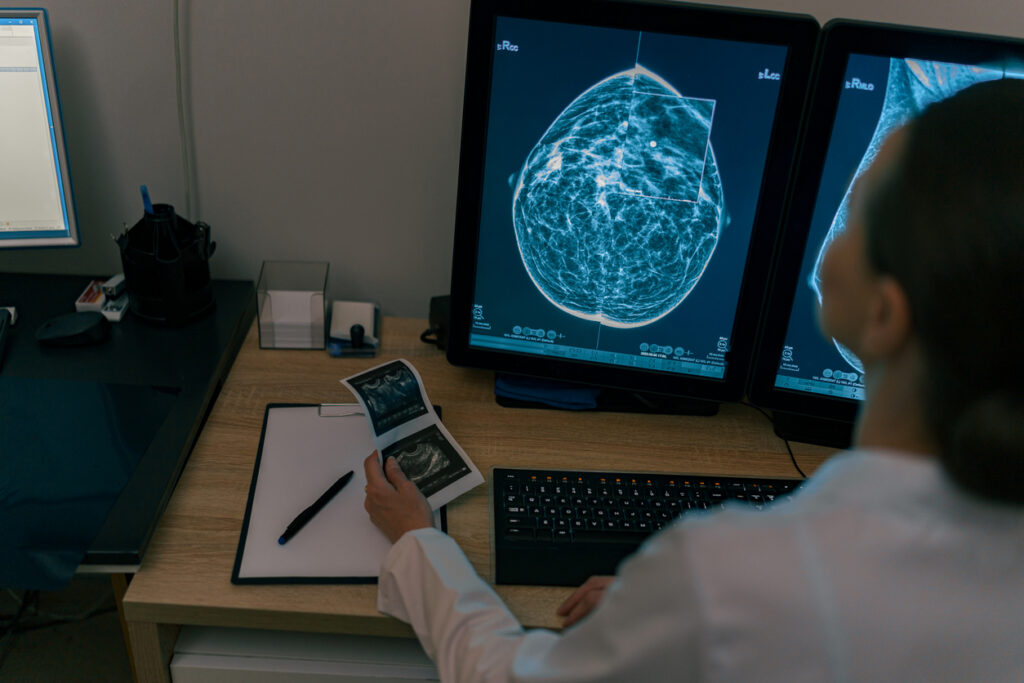
What Breast MRI Is
Breast MRI (magnetic resonance imaging) uses powerful magnets and radio waves to produce highly detailed images of breast tissue.
During the exam, patients lie on a table that slides into the MRI scanner. A contrast dye is often injected into the bloodstream to improve visibility of blood flow and tissue abnormalities.
Who May Benefit From Breast MRI
Medical professionals typically recommend breast MRI for women at higher-than-average risk of breast cancer.
This may include individuals who:
- Have a strong family history of breast cancer.
- Carry certain genetic mutations (such as BRCA1 or BRCA2).
- Previously received chest radiation therapy at a young age.
Healthcare providers often use MRI screening alongside mammography for high-risk patients to improve early detection.
Understanding Breast Density
Breast density refers to the amount of fibrous and glandular tissue compared to fatty tissue in the breasts.
Women with dense breast tissue have a higher proportion of glandular tissue. Dense tissue looks white on a mammogram, which is similar to how tumors look. This makes it harder to find cancer.
Dense breast tissue is common and not abnormal, but it can make screening more challenging. For this reason, doctors may recommend additional imaging tests, such as an ultrasound or MRI, for some patients with dense breasts.
Women who have questions about their breast density should discuss screening options with their healthcare provider.
Breast Cancer Screening Guidelines
Screening recommendations vary slightly among medical organizations, but general guidelines often include:
Ages 40–44
Women may begin annual mammograms based on personal preference and physician guidance.
Ages 45–54
Healthcare providers typically recommend annual mammograms.
55 and older
Screening may continue every one to two years, depending on health history and physician recommendations.
Some individuals may require earlier or additional screening if they have risk factors such as:
- Family history of breast cancer
- Genetic predisposition
- Dense breast tissue
- Prior abnormal imaging results
A personalized screening plan ensures each woman receives the most appropriate care.
Preparing for a Breast Imaging Appointment
Preparing for a breast imaging exam can help ensure accurate results and a smoother experience.
Patients should consider the following tips:
- Wear comfortable clothing: two-piece outfits make it easier to change for the exam.
- Schedule wisely: Many women prefer scheduling mammograms when their breasts are least tender, such as the week after their menstrual period.
- Avoid lotions and deodorants: Products applied to the underarms or chest area may appear on imaging and interfere with results.
- Bring prior imaging records: Patients should bring previous mammograms to a new imaging center so radiologists can compare images over time.
Understanding Your Breast Imaging Results
After a breast imaging exam, the images are reviewed by a radiologist who specializes in interpreting medical imaging.
Results are typically reported using a standardized system called BI-RADS (Breast Imaging Reporting and Data System). This system categorizes findings to help guide follow-up care.
BI-RADS categories range from:
- Category 0: Additional imaging needed.
- Category 1: Negative (no abnormal findings).
- Category 2: Benign findings.
- Category 3: Probably benign, follow-up recommended.
- Category 4–5: Suspicious findings that may require biopsy.
In many cases, additional imaging simply provides clearer views and does not necessarily indicate cancer.
When to Talk to Your Doctor About Breast Screening
While routine screening is essential, patients should also contact their healthcare provider if they notice any changes in their breasts.
These may include:
- A new lump or thickening in the breast.
- Changes in breast shape or size.
- Skin dimpling or redness.
- Nipple discharge or inversion.
Individuals with a family history of breast cancer should also discuss risk factors and screening options with their doctor.
Open communication with a healthcare professional ensures appropriate screening and timely evaluation of any concerns.
Schedule Your Breast Screening
Regular breast screening plays a critical role in protecting long-term health. By detecting potential problems early, imaging tests help doctors provide timely care and improve treatment outcomes.
Whether through mammography, ultrasound, or MRI, modern breast imaging technologies offer powerful tools for identifying abnormalities and monitoring breast health.
If it has been a while since your last screening, or if you are unsure when to begin, talk with your healthcare provider about scheduling your next breast imaging appointment. Regular screening offers peace of mind and is a necessary step toward early detection.
Reach out to us today to get started!