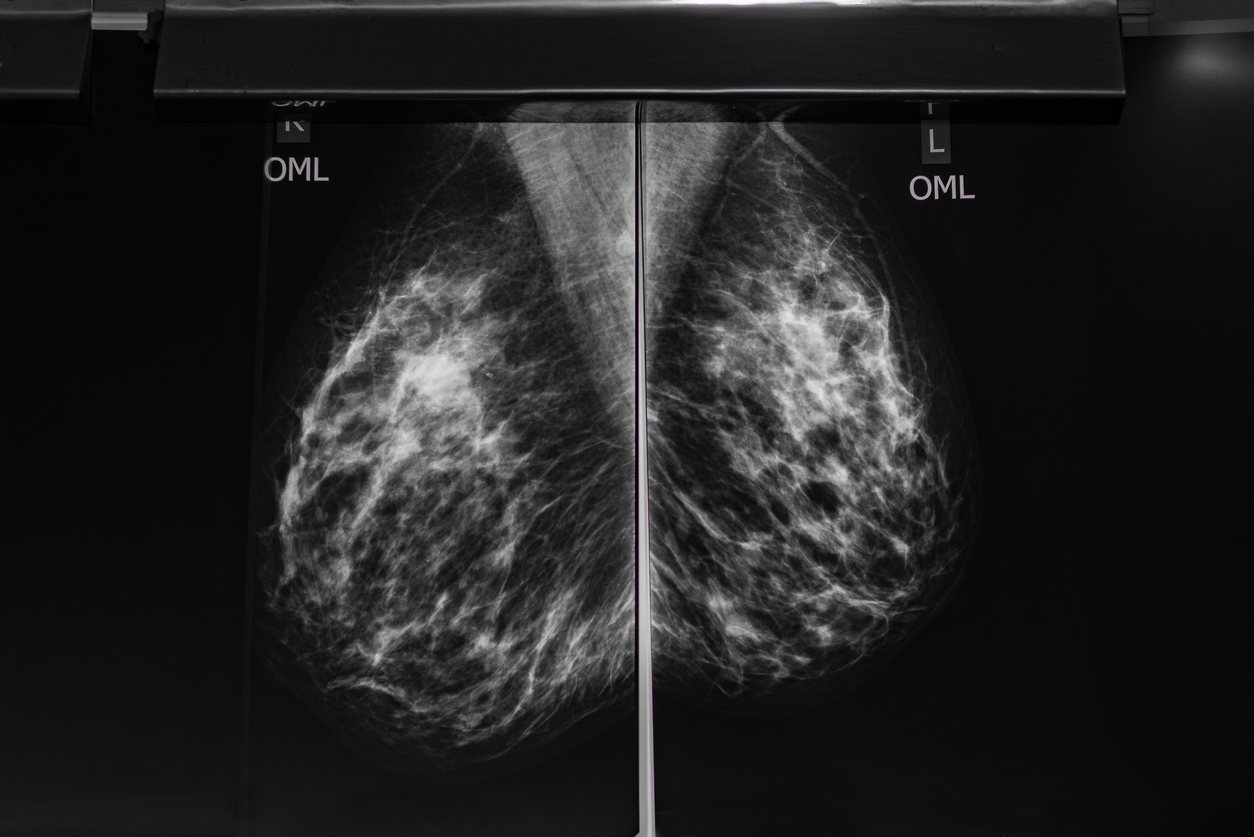
Breast cancer screening is one of the most significant tools for early detection and improved treatment outcomes. While most people are familiar with mammograms, fewer understand how dense breast tissue can influence screening results and follow-up care.
Breast density refers to the composition of breast tissue as seen on a mammogram. It does not describe how breasts feel during a physical exam but rather how different tissues appear on imaging.
Understanding what dense breast tissue means and how it affects breast cancer screening can help patients make more informed decisions about their health. This guide explains breast density, shows why it affects screening, and recommends when to consider additional imaging.

What Breast Density Means
Several types of tissue make up the breasts. The two primary categories are
Fatty Tissue
Fatty tissue appears darker on a mammogram and is easier for radiologists to see through when evaluating breast images.
Dense Tissue (glandular and connective tissue)
Dense tissue includes milk glands, ducts, and supportive connective tissue. On a mammogram, dense tissue appears white. Breast density refers to the relative amount of these tissues present in the breast. Imaging determines breast density, not how the breasts look or feel.
A person cannot determine their breast density through self-exam or physical appearance. Dense breasts are also very common. Research shows that about 40–50% of women who undergo mammograms have dense breast tissue.
Radiologists typically classify breast density into four categories:
- Mostly fatty tissue
- Scattered areas of fibroglandular density
- Heterogeneously dense tissue
- Extremely dense tissue
Doctors generally consider the last two categories ‘dense.’
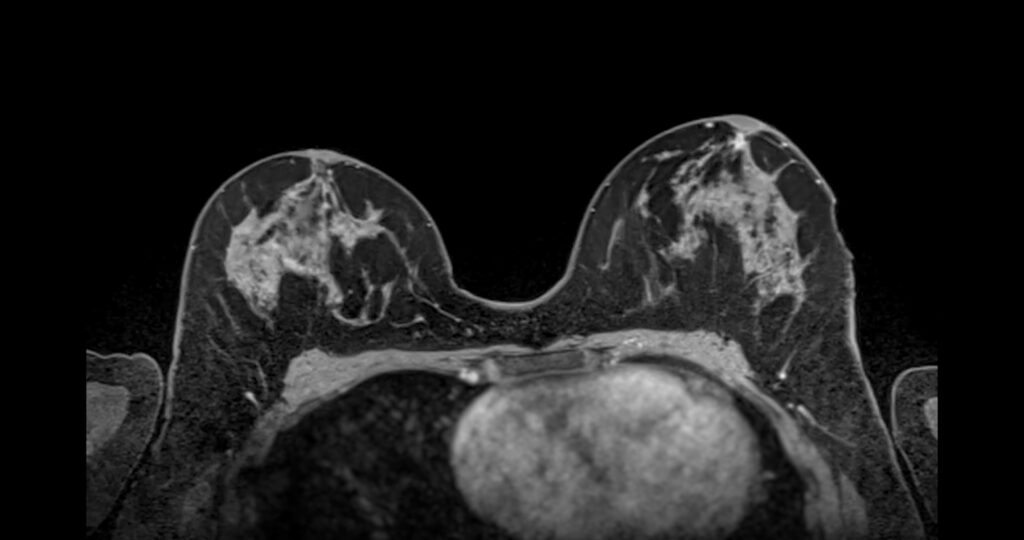
Why Dense Tissue Can Make Cancer Harder to Detect
Dense breast tissue matters primarily because it can affect how easily cancer appears on a mammogram.
Both dense tissue and tumors show up white on mammogram images. Because they appear similar in color, dense tissue can sometimes make it more difficult for radiologists to detect abnormalities.
A common analogy doctors use is that finding cancer in dense tissue is like trying to spot a snowball in a snowstorm; similar colors make subtle differences harder to see.
This does not mean mammograms are ineffective for women with dense breasts. Mammography remains the most important and widely recommended breast cancer screening tool.
According to the American College of Radiology, mammograms are still highly effective at detecting many breast cancers and remain the foundation of breast screening programs. However, in certain cases, doctors may recommend additional imaging to provide a more complete picture of breast health.
Why Additional Imaging May Be Recommended
For some individuals with dense breast tissue, physicians may recommendsupplemental imaging alongside standard mammography.
Additional screening tools can help provide more detailed images or reveal abnormalities that may be less visible on a standard mammogram.
Common supplemental imaging options include:
3D Mammography (Digital Breast Tomosynthesis)
3D mammography is an advanced imaging technique that captures multiple X-ray images from different angles around the breast. The system reconstructs these images into a layered, three-dimensional view of breast tissue.
Radiologists can examine the tissue one layer at a time, improving detection of small cancers that dense tissue might hide. 3D mammography also reduces false positives and the need for repeat imaging.
Breast Ultrasound
Breast ultrasound uses sound waves to produce images of the breast rather than radiation.
It is often used as a supplemental screening tool for women with dense breasts. Ultrasound can help identify abnormalities that may not be clearly visible on a mammogram.
This imaging method is also useful for distinguishing between solid masses and fluid-filled cysts.
Breast MRI
Breast MRI (magnetic resonance imaging) is one of the most sensitive imaging methods available for detecting breast cancer.
MRI uses powerful magnets and radio waves to create detailed images of breast tissue. A contrast agent is typically used to highlight areas with increased blood flow, which may indicate abnormal tissue.
Breast MRI is generally recommended forpatients at higher risk of breast cancer, including those with strong family histories or known genetic mutations. According to the National Comprehensive Cancer Network, MRI screening may be used alongside mammography for individuals with elevated risk factors.
The decision to use additional imaging depends on several factors, including:
- Personal medical history
- Family history of breast cancer
- Genetic risk factors
- Age
- Physician recommendations
Each patient’s screening plan should be personalized based on their individual risk profile.
New Federal Breast Density Notification Rules
In recent years, breast density awareness has become an important focus in healthcare policy. New federal regulations in the United States now require mammography providers to inform patients about their breast density in their mammogram reports.
This rule ensures that women receive clear information if they have dense breast tissue. The notification typically explains:
- Whether the patient has dense breasts.
- That dense tissue can make cancer harder to detect on mammograms.
- That additional imaging may sometimes be helpful.
The goal of this requirement is to encourage informed conversations between patients and their healthcare providers.
Understanding breast density empowers patients to ask questions and explore whether additional screening may be appropriate for them.
When to Talk to Your Doctor
If you learn that you have dense breast tissue, it is a good idea to discuss your screening options with your healthcare provider.
Your doctor can help evaluate your individual risk and determine whether additional imaging may be beneficial.
Topics worth discussing include:
- Your breast density: Ask your doctor how your density level may affect screening and detection.
- Personal risk factors: Factors such as family history, genetic mutations, or previous abnormal screenings may influence your screening plan.
- Whether supplemental imaging is appropriate: Depending on your risk level, your physician may recommend additional tests such as ultrasound, 3D mammography, or MRI.
These conversations help ensure that screening strategies are tailored to each patient’s specific needs.
If you are due for routine imaging, you can also schedule an appointment to get a mammogram screening and review your results with a medical professional.
Regular screening combined with informed decision-making provides the best protection for long-term breast health.
Being Proactive in Your Health and Wellness
Dense breast tissue is common and affects nearly half of women undergoing mammograms. While it can make breast cancer slightly more difficult to detect on imaging, it is an important and manageable factor in breast health.
The most essential step patients can take is to continue regular screening and stay informed about their individual risk factors. Modern breast imaging technologies, including mammography, ultrasound, and MRI, allow doctors to evaluate breast tissue more effectively than ever before.
By understanding dense breast tissue and maintaining open communication with healthcare providers, patients can ensure they receive the most appropriate screening and care. Regular exams, informed discussions, and personalized screening plans all play an essential role in early detection and long-term peace of mind. Reach out to our healthcare team and get a mammogram screening scheduled today!